What is Arthritis?
Arthritis, actually, is not a single disease; it is an informal way of referring to joint pain or joint disease. According to the Arthritis Foundation, there are more than 100 types of arthritis and related conditions. People of all ages, genders and races can have arthritis, and it is the leading cause of disability in America. More than 50 million adults and 300,000 children have some type of arthritis. It is most common among women and occurs more frequently as people get older.
Common arthritis joint symptoms include swelling, pain, stiffness and decreased range of motion. Symptoms may come and go. They can be mild, moderate or severe. They may stay about the same for years but can then progress or get worse over time. Severe arthritis can result in chronic pain, an inability to do daily activities and may make it difficult to walk or climb stairs.
Arthritis can cause permanent joint damage. This damage may be visible, such as knobby finger joints, but often it can only be seen by x-rays. Some types of arthritis also affect the heart, eyes, lungs, kidneys and skin as well as the joints.
What causes arthritis?
Wonder what causes arthritis. Why do you suffer with it but others in your family do not? Many things can cause different types of arthritis. For example, osteoarthritis is caused by the breakdown of cartilage, a rubbery material that eases the friction in your joints. Part of the cartilage thins and the surface becomes rougher. Then the joint doesn’t move as smoothly as it should. When cartilage becomes worn or damaged, all the tissues within the joint become inflamed as the body tries to repair the damage. However, the repair processes don’t always work so well and changes to the joint structure can sometimes cause even more inflammation, resulting in symptoms such as pain, swelling or difficulty in moving the joint normally.
Uric acid crystals, which form when there’s too much uric acid in your blood, can cause gout. Most of the time, a high uric acid level occurs when your kidneys don’t eliminate uric acid efficiently. This can be caused by eating rich foods, being overweight, having diabetes, taking certain diuretics (sometimes called water pills) and drinking too much alcohol. Gout is a common and complex form of arthritis that can affect anyone. It’s characterized by sudden, severe attacks of pain, swelling, redness and tenderness in one or more joints, most often in the big toe.
Rheumatoid arthritis or RA is a chronic inflammatory disorder affecting many joints, in which the immune system attacks the joints (beginning with the joint lining) including those in the hands and feet. As with other autoimmune diseases, researchers think that certain genes may increase your risk of developing RA. But they also don’t consider RA an inherited disorder. This means that a geneticist can’t calculate your chances for RA based on your family history.
Infections or underlying disease, such as psoriasis or lupus, can cause other types of arthritis.
What are some all-natural remedies for reducing arthritis pain?
If you are looking for a natural way to overcome arthritis pain, there are many options to consider. Experts recommend lifestyle changes to help ease arthritis pain. Many “home remedies,” including losing weight and certain kinds of non-impact exercises like Tai-Chi, swimming, or yoga, can be helpful. Others recommend adding Vitamin D, and omega-3 fatty acids for reducing inflammation. And dietary experts say eating foods with plenty of omega-3s, including nuts, seeds, and cold-water fish, may also help to reduce inflammation.
Chiropractic help for arthritis pain
When diet and exercise are not enough or if you are suffering from severe arthritis pain, you may want some other natural options. First of all, a visit to a good chiropractor would be smart. A chiropractor may gently manipulate your soft tissue to stop muscle spasms and relieve tenderness. He or she may use active exercises or traction to slowly stretch your joints and increase your range of motion. Your visit may feel like a more hands-on version of physical therapy.
Chiropractic care is a very safe and effective method of treating arthritis pain. No drugs are used since they only suppress the symptoms of arthritis without addressing the cause. Instead, chiropractic adjustments can help naturally reduce joint restrictions or misalignments to reduce inflammation.
Pressure Point Therapy for Arthritis Pain
Another effective recommended treatment option is ]Pressure Point Therapy. This type of therapy involves relieving “pressure points” — painful knots of energy located on your body’s nerve pathways. These knots prevent the normal flow of energy along your nerves which can mean problems such as stiffness, soreness and an inability to move the way you would like. Pressure Point Therapy, also known as Trigger Point Therapy, helps to relieve these problems.
Pressure Point Therapy is a perfect companion to chiropractic care. Chiropractic adjustments will shift the spinal vertebrae so they are in better alignment, but your muscles may need to adjust to these new positions. By combining Pressure Point Therapy with chiropractic adjustments, your muscles will adjust more quickly. Any nerves that were irritated by those misaligned vertebrae can relax, almost as if they are breathing a sigh of relief.
If you are suffering from arthritis pain, we can help — just call for an appointment at (758) 518-5000.
Arthritis means joint inflammation and there are over 200 different types of arthritis that can affect both young and old people.
Arthritis can affect different parts of the body and each type has a different cause. It is a group of conditions involving damage to the joints and in some cases can also affect the soft tissues of the body such as ligaments, lungs and heart valves.
The most common forms of arthritis are osteoarthritis (OA), rheumatoid arthritis (RA), psoriatic arthritis, ankylosing spondylitis (AS), gout and systemic lupus erythematosus (SLE).
Arthritis is the leading cause of disability in people older than fifty-five years.
- Most arthritic conditions benefit greatly from Chiropractic treatment and should be considered as an adjunct to medical care, particularly osteoarthritis, which is the most common type of arthritis.
- Osteoarthritis is often treated with anti-inflammatory medication and nothing else. This is a mistake. Using anti-inflammatory medication in the long term has been shown to impair the healing rate of cartilage and can also cause damage to the lining of the stomach and result in fatal stomach bleeds, particularly in the elderly. Fortunately there are better ways to manage osteoarthritis.
- If you receive chiropractic treatment, including laser treatment, regular, gentle exercise and improve your diet, you can reduce your need to take anti-inflammatory medication, which is great news. In fact some of our patients have been able to stop taking them all together. Read more about chiropractic treatment.
- With regard to the inflammatory arthriditis, such as rheumatoid arthritis (RA), psoriatic arthritis and ankylosing spondylitis (AS), there is not a real cure for these conditions.
- Although, they have their natural peaks and troughs, the inflammatory process can be quite severe and it is therefore important to take medication to control it to avoid joint destruction. Chiropractic treatment is still useful as a therapy for these conditions to help you control the symptoms.
- The following pages will help you get more of an understanding of the different types of arthritis, which symptoms are expected, how they are diagnosed and treated.
- What is Osteoarthritis?
- What is Rheumatoid Arthritis?
- What is Ankylosing Spondylitis?
- What is Juvenile Rheumatoid Arthritis (Still’s disease)?
- What is Psoriatic Arthritis?
- What is Gout?
- What is Systemic Lupus Erythematosus?
Osteoarthritis is a degenerative joint disease and occurs as the result of wear and tear. It mainly affects the weight-bearing joints e.g. the spine, hips, knees, ankles and joints in the hands. It can affect both men and women at any age, but is more common as we get older. Osteoarthritis has many names, Arthritis, spondylitis, rheumatism or rheumatics are names given to the pain and stiffness resulting from it.
Degeneration of your joints begins without you knowing and it happens slowly to all of us.
The general wear and tear of a lifetime results in joints laying down extra areas of bone in an attempt to support damaged areas. Generally our bodies compensate for this and we feel no pain up to point.
However, loss of movement in a joint wear of the joint cartilage will eventually cause you pain. It might come and go and then becomes more constant.
Chiropractic cannot stop you getting old, but it might stop you feeling it!
The symptoms of arthritis are commonly treated with non-steroidal anti-inflammatory drugs (NSAIDs), which don’t stop the progression of the disease and have risks associated, but sometimes help to relieve the pain.
However, chiropractic treatment is considered by some people to be more effective in the long run.
It has been suggested that chiropractic can prevent further arthritic development and regular treatment can even prevent osteoarthritic changes occurring in the first place. All we know for sure is that many of our patients say that it helps them feel better and are able to stay more active and take care of themselves better.
There is no real strong evidence that degeneration of your joints cannot be reversed but your chiropractor can help improve muscle and joint function and therefore reduce the symptoms of arthritis.
Along with chiropractic treatment, greater emphasis is now being placed on a controlled and regulated diet to reduce joint inflammation and arthritic pain.
Many elderly patients participate in spinal rehabilitation with specially modified exercise programmes.
Ageing of the Spine
During our lifetime, our spines are required to withstand considerable weight-bearing stresses resulting from activities of daily living.
As a result of these stresses ‘wear and tear’ or degeneration, occurs in all parts of the vertebral column. Degeneration which occurs in the spine as a consequence of daily living is considered part of the normal ageing process.
The intervertebral discs (IVDs) are the first to undergo changes, usually around the age of 40, followed later by the spinal joints and bony vertebra, form the ages of 50-60 onwards. Normal degeneration is usually well-established by the age of 70.
Characteristically, the IVD will lose its ability to absorb fluid as the chemical makeup and internal architecture of the disc changes in response to repetitive stresses.
As a result, the normally resilient disc will become tougher, more fibrous and less able to respond to weight-bearing load. The ageing of the discs puts greater stress on the spinal joints as well as the vertebrae itself.
The overall effect of degenerative changes in the disc, joints and bony vertebrae leads to the characteristic feeling of stiffness and reduced movement of the spine.
Degeneration of your joints cannot be reversed but your chiropractor can help improve how you feel and allow you to live life to the full.
What is Rheumatoid arthritis?
Rheumatoid arthritis (RA) is a specific type of arthritis that is chronic, progressive and often debilitating, characterised by the symmetrical joint involvement and the age at which it begins.
It differs from the more common osteoarthritis (OA) often known as wear and tear, spondylosis, degenerative joint disease (DJD) or rheumatism. It can also affect other parts of the body such as the heart, lungs, small blood vessels, the nervous system and eyes. When this occurs, it is referred to as rheumatic disease. Any type of arthritis involves inflammation which can cause redness, swelling, stiffness, pain, loss of joint function and eventually joint deformity.
With RA, an auto-immune response – (the body’s immune system starts to attack itself) causes damage to certain joints. The body’s white blood cells (immune defence system) cannot differentiate from bad cells and its own body cells. Nobody knows what causes or triggers RA, but it has long been believed that infectious agents such as bacteria, viruses and fungi are involved in starting the inflammatory chain of events, although none have been proven as yet.
Some scientists believe that certain environmental factors can trigger the inflammation to start, and that there is a hereditary link to RA with genetic make-up influencing who is susceptible to it.
Who is affected by Rheumatoid arthritis?
RA affects two to three times more women than men and typically occurs between the ages of 25 and 50 years of age, although the onset can vary to affect children as young as six months old as with juvenile rheumatoid arthritis (Still’s disease)? also known as juvenile idiopathic arthritis (JIA).
The joints affected by rheumatoid arthritis differ to those affected by osteoarthritis due to the nature of the disease. OA affects the weight bearing joints, which become more prone to erosion through wear and tear. The affected joint distribution is usually non-symmetrical and can affect the whole spine.
With RA, it is the synovial joints (specific type of joint) that are affected. The distribution tends to be symmetrical – with the most common joints affected being the smaller joints of the hands and feet, although it can affect any synovial joint. RA for example will tend to affect the smaller joints of the hands and wrists away from the fingernails, where as OA will favour the joints closest to the fingernails.
To date, no-one really knows why some joints are affected over others with RA. In the past, some theories have included an increased blood supply being responsible for targeting the specific joints, although to date, these have not been proven.
How a normal joint works
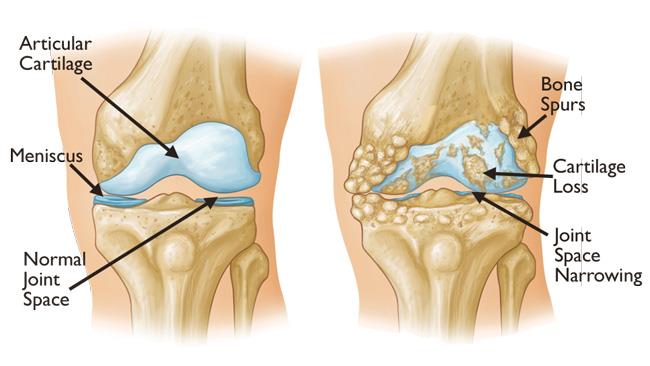
In a normal joint, the bone surfaces are lined with cartilage, which acts to reduce friction and helps absorb the stresses that are placed on the joint in everyday situations.
Surrounding the joint is a very thin membrane (called the synovial membrane or synovium) that produces synovial fluid, and acts like a sac. This fluid is important in providing the nutrients needed to feed the cartilage to make sure it is healthy and provides as much lubrication as possible within the joint. Encapsulating the joint and synovium is the joint capsule – a tough coating which keeps everything together – to which ligaments and tendons surround, providing stability and movement to the joint. Damage to any of these structures can result in pain and swelling around the joint with a potential loss of function depending on the structure that has been injured.
In Osteoarthritis, as a result of repeated stresses and shock absorbing, the joint space starts to narrow and the cartilage within the joint starts to wear away, becoming damaged. It becomes thinner and no longer provides as much lubrication as before. The joint surfaces therefore start to rub, causing irritation and pain which in turn causes inflammation and swelling. The bone surfaces react to this change by laying down more bone often in the form of spurs at the end of the bones themselves. The joint becomes deformed as a result causing further pain and stiffness, and loss of normal movement. These changes can be seen on X-Ray as a narrowing of the normal joint space, changes in the bone density (areas of increases whiteness) directly at the joint and bony spurs (osteophytes) present on the outer margins of the affected joints.
In Rheumatoid Arthritis, usually an infection or incident will trigger the body’s immune system to attack its own tissues and start the inflammatory process. The white blood cells infiltrate the synovium surrounding the joints causing them to become inflamed. This causes an excess production of fluid within the joint itself and thickening of the synovial membrane (pannus formation). Pannus progresses to spread throughout the whole joint and starts to erode away the cartilage covering the ends of bone, and eventually the bone surfaces which ultimately results in the deformation of the joint. The changes can be seen on X-ray as the bone surfaces and margins are eaten away.
The symptoms of RA can vary from person to person. When the disease is active, the tissues are inflamed. When the disease is in remission, the inflammation has eased and the symptoms disappear with patients generally feeling well. Remissions can occur spontaneously or with treatment and can vary in length between weeks and years in duration. When the disease becomes active again the symptoms return. The first symptoms of RA can start as pain, swelling and stiffness in one or more of the same joints in both sides of your body (symmetrical distribution). They can start suddenly (acute onset) or more commonly, over a longer period of time (insidious onset). The morning joint stiffness lasts considerably longer than 30 minutes and is often accompanied with poor sleep due to waking up in the middle of the night from the joint pain and stiffness. Patients will often experience fatigue, weight loss and generally feel unwell or have flu-like symptoms.
Other parts of the body can also be affected, although this doesn’t happen with everyone. The inflammation of RA can cause swelling under the skin in the form of rheumatic nodules – firm, non-tender nodules under the skin present in approximately 25% of patients with RA. These typically occur at bony areas where there is frequent pressure such as the elbows, but can also occur elsewhere in the body including the internal organs. Even though these do not cause any symptoms, they can occasionally become infected. RA patients can also develop inflammation of the membranes surrounding the internal organs such as the heart causing pericarditis, nodules and ischaemic heart disease. In some cases, the lung tissue becomes inflamed (pleuritis), causing again nodules and fibrosis. Inflammation of the tear glands in the eyes and salivary glands in the mouth is often referred to as Sjögren’s syndrome and will result in dry eyes and mouth. Rarely, inflammation can affect the blood vessels (vasculitis) causing problems with the skin in the form of ulcers and the nerves. It is usually visible as tiny black areas around the nail beds or as leg ulcers.
Diagnosis of Rheumatoid arthritis
Your GP and usually a consultant rheumatologist (joint specialist) are required to confirm the diagnosis and will base it on whether a certain number of criteria have been filled. These may be less obvious during the early stages of the disease, but can be confirmed with blood test results.
A specific marker within the blood (rheumatoid factor or RF) is often present in RA and a selection of other inflammatory conditions such as Sjorgen’s syndrome, dermatomyositis, scleroderma, systemic lupus erythematosus (SLE). However, if RF is not present it does not necessarily mean that you do not have RA, and likewise, if you do have RF it does not necessarily mean that you have RA. There are two different types of RA – sero-positive RA when RF is present in the blood, and sero-negative RA when RF is not present in the blood. However, the type of RA does not influence the treatment in any way – it is used as a diagnostic aid for the diagnosing physician.
Below are the criteria that must be present for at least six weeks for a diagnosis of RA to be made:
- Stiffness in and around the joints lasting for at least 1 hour in the morning
- Swelling in the area surrounding the joints in three or more joint areas at any one time
- Swelling of the first finger (proximal interphalangeal), hand or wrist joints
- Symmetrical swelling.
Once diagnosed with RA, the physician needs to determine at what stage of the disease you are in to come up with the most effective treatment plan and rehabilitation program. This is usually defined through the presence of rheumatic nodules, rheumatoid factor and x-ray changes.
Treatment and management of Rheumatoid arthritis
Due to the nature of the condition, the focus of the treatment is to suppress the joint damaging process. This is usually achieved through medication to control the inflammation and disease progression and is usually administered in the form of DMARDs, steroids and biologic agents. In advanced cases where medication is not sufficiently controlling the joint damage, surgery might be required to deal with structural changes.
An early diagnosis is important to minimise the amount of joint damage and complications that can occur with RA and improve the quality of life.
Once under control, there are several ways to ease the symptoms. These include:
- education about the condition and support to patients with RA and their families,
- non-drug treatments including topical treatments and pain relieving strategies (rest and relaxation),
- physical therapy such as chiropractic and occupational therapy,
- pain-killers and non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen,
- immuno-supressants
- joint injections and
- pain management clinics.
Can chiropractic help?
Chiropractic treatment is concerned with the diagnosis, treatment and prevention of disorders of the neuro-musculoskeletal system. This means we focus mainly on the nervous system, the muscles and joints of the body and aim to make them work as well as they possibly can do.
Having taken a full and thorough history and completed a full examination, your chiropractor will discuss the treatment options with you and how best to optimise the care given in between treatments.
This may be in the form of mobility, strengthening and supporting exercises, icing and heat advice, and advice in a choice of supporting aids as part of the multi-professional care team needed for patients with RA.
The Chiropractic management itself will focus on easing the stiffness in joints built up from immobility and lack of use from pain, and relaxing tight muscles aimed at maximising joint function and mobility.
The techniques used will vary depending on your individual circumstances and presentation as not all types of treatment are appropriate for everyone. The use of a Low Level Laser Therapy or cold laser has been shown to be effective in controlling inflammation and improve healing.
Psoriatic (Sor-ee-at-tic) Arthritis is an autoimmune inflammatory arthritis, similar to Rheumatoid Arthritis, but with a negative RA factor. When we talk about ARTHRITIS, most people think of the good old fashioned wear and tear arthritis where the joint has lost it’s cartilage or lubricating factor, so that it’s bone on bone grinding. This kind of arthritis is known as OSTEO Arthritis.
There is another kind of arthritis, at the other end of the spectrum, called INFLAMMATORY ARTHRITIS. These are the AUTO-IMMUNE types of arthritis where your body attacks it’s own tissue, thinking your own tissue is a foreign invader. The immune system goes in to over-drive as it attempts to fight what it thinks is a bacteria or virus. White blood cells flood the area, in this case the joint, and this creates inflammation, which causes swelling, redness, heat and pain. In this realm of inflammatory arthritis, there is a further separation into two categories. On the one side is the Rheumatoid Factor, RF or RA positive, which includes Rheumatoid Arthritis, Systemic Lupus, Scleroderma, etc. On the other side is the “Negative RA Factor” side, meaning there is no RF antibodies present and is called SPONDYLO-ARTHRITIS (spon-de-low). The blood test that indicates this side of inflammatory arthritis is called HLA-B27 (Human Leukocyte Antibody) and includes the inflammatory arthritis categories as Psoriatic Arthritis, Ankylosing Spondylitis, Enteropathic Arthritis, and Reactive Arthritis.
Managing Arthritis In Dublin, Ireland
Psoriatic Arthritis (PsA) is a long-term inflammatory joint disease that may cause swollen and painful joints, skin lesions, and fatigue. If you are one of the many people who suffer from PsA, you know how frustrating and debilitating it can be.
Thankfully, there are treatments available to help manage PsA and improve your quality of life.
Dublin Physical & Chiropractic offers a variety of treatments specifically designed to help those with Psoriatic Arthritis. We have years of experience in helping people just like you get relief from their symptoms.
Contact us today to learn more about our services.

What Causes This Form Of Arthritis?
Psoriatic arthritis is an immune-related illness. PsA is believed to be a genetic disease that triggers the body’s immune system to attack healthy tissue, causing inflammation and damage in multiple areas of the body, including joints and skin.
Psoriatic arthritis affects about 30 percent of people with psoriasis (a common skin condition).
Psoriasis And Psoriatic
Psoriasis causes patches of red, scaly skin. Psoriatic arthritis is more common in people who have a family history of the disease.
What Are The Risk Factors? Psoriatic Arthritis Diet
There are two main risk factors, along with having psoriasis:
- Age: Psoriatic arthritis typically occurs between the ages of 30 to 35.
- A family history of psoriatic arthritis.
- Diet: Increased weight is associated with psoriasis.
Psoriatic Arthritis Symptoms
The symptoms of psoriatic arthritis can vary from person to person and change over time. Some people may experience only mild symptoms while others may have severe PsA.
Symptoms may include joint pain, swelling, stiffness, and tenderness of the joints. Psoriatic Arthritis can affect any part of your body including:
- Fingers
- Toes
- Wrists
- Elbows
- Ankles
- Knees
PsA may also cause fatigue, a low-grade fever, and changes in mood.

How Is Psoriatic Arthritis (PsA) Diagnosed?
There is no definitive test for diagnosing psoriatic arthritis. A doctor will likely ask about your medical history and do a physical examination. He or she may also order tests such as:
- Blood tests (to check for inflammation)
- X-rays, MRIs, or CT scans to look at the affected joints and tendons.
Psoriatic arthritis is often misdiagnosed as rheumatoid arthritis, osteoarthritis, or gout because they share many of the same symptoms.
It is important to see a doctor who is familiar with PsA and can make an accurate diagnosis.
Treatment Of Psoriatic Arthritis In Dublin, Ireland
Suffering from psoriatic arthritis? You’re not alone.
Millions of people around the world suffer from psoriatic arthritis, and our team of experts specializes in providing an optimal treatment plan for this condition. We offer a range of evidence-based innovative treatment options that have helped many people achieve relief from their symptoms.
Our treatment options are drug-free, non-surgical interventions, and are tailored to you. You can be confident that we will work with you to develop a treatment plan that meets your specific needs and goals.
Contact us today to schedule a consultation and learn more about how we can help you manage your psoriatic arthritis.
How Do We Help People With This Form Of Arthritis
We use a combination of chiropractic, physical therapy, and other treatment modalities that are highly effective in Psoriatic Arthritis.
Chiropractic Care For Arthritis
A chiropractor will evaluate your spine, joints, tendons, and ligaments to determine if there is a misalignment of the vertebrae or injury to any of the components that make up the spine. Psa often affects areas such as the lower back, shoulder, and neck.
If there is misalignment or injury to these structures, a chiropractor will use a series of manual adjustments in an effort to restore alignment and improve mobility. Chiropractic treatment can help reduce pain and inflammation associated with PsA and improve mobility.
Physical Therapy Care
A physical therapist uses a variety of techniques to help reduce pain and inflammation associated with PsA, as well as improve strength and flexibility in joints that have been affected by PsA.
Physical therapy can include stretching, exercise therapy, massage therapy, and laser therapy.
Laser Therapy For Psoriatic Arthritis
We use a Class IV laser at Dublin Physical & Chiropractic. It is highly effective for reducing pain, swelling, and inflammation of arthritic joints, to allow freedom of movement and improved range of motion.
Laser therapy is also effective for skin conditions.
Laser therapy uses light therapy to increase cellular activity, speed up the recovery process, and promote cellular regeneration.
Ankylosing Spondylitis (AS) and Chiropractic Treatment
Ankylosing Spondylosis is an inflammatory disease affecting mainly the pelvic (sacroiliac) joints, spine and rib joint, causing pain and progressive stiffness.
It affects young male about four times as often as female. Onset typically occurs between the ages of 15 to 45
Symptoms Of Ankylosing Spondylitis
The main presenting complaints in the early stages are lower back pain with morning stiffness that often wares off during the day with activity. In some cases the inflammation can be so severe that the pain is constant and severely disabling, but this is rare.
The pain and stiffness can progress to affect the mid back and neck, and in about a quarter of people with AS it affects the joints in the limbs, with the hips being the most common, affecting half the people with AS.
If the chest and ribs are affected, it can make it difficult to take a deep breath. The legs can become weak and numb if certain nerves are pinched or trapped but this is very rare.
What Is Ankylosing Spondylitis?
The exact cause is not fully understood but it is classified as an autoimmune disorder, which means that the body’s immune system is attacking some of its own cells causing ongoing inflammation. It is classified as one of the so-called sero-negative arthropathies (the rheumatoid factor is not present).
As it progresses, ossification is triggered by the body’s defense mechanism. Ossification causes new bone to grow along the ligaments between vertebrae gradually limiting movement and eventually fusing them together. Further, ossification may affect spinal ligaments causing narrowing of the spinal canal (central stenosis), which can result in compression of nerves but this is very rare.
What Tests Will The Chiropractor Do To Confirm AS?
Case history and Examination
The chiropractor will first of all review your general health and family medical history. It is important for the chiropractor to know if any family member has had the problem.
A family history of Ankylosing Spondylitis may be indicative in diagnosing this condition, but it is not necessary.
During the physical examination, you will be asked to move and bend in different ways so the chiropractor can see how flexible your spine is.
In the early stages subtle changes can be significant. In a later stage the mobility can be significantly reduced.
The chiropractor will also check your chest expansion which can be reduced in AS.
The chiropractor will also do a neurological examination.
X-ray Examination
If the findings in the history taking and examination suggest that you may have AS, the chiropractor will take X-rays.
The signs on X-rays are usually quite characteristic and if the findings correlate with the history and examination, a diagnosis can often be made with good accuracy.
There are very characteristic signs on x-rays that the chiropractor can look for.
In the early stages there is a widening of the pelvic (sacroiliac) joints (SI) with irregularity of the joint surface and sclerosis (whitening of the bone). There may be squaring of the vertebrae and mild calcification of the outer part of the discs (causing what is called ‘shiny corner signs’ and syndesmophytes).
In the later stages when the condition has been present, usually for many years, fusion may occur causing a so called ‘bamboo spine’.
A CT- or MRI-scan may be ordered to see the spine in greater detail, especially if the x-rays do not correlate with the findings in the history and examination.
However, we would inform your GP and normally suggest that you have blood tests taken to support the diagnosis.
Blood Tests
A blood sample is taken to look for an antigen called HLA-BA27, which is positive 96% of the time. But the presence of HLA-BA27 does not mean that you have AS for sure. It is just an indicator that you may have it. (An antigen is a protein that helps the body to make antibodies to fight infection.)
Blood tests are usually negative for rheumatoid factor, which will rule out Rheumatoid arthritis.
ESR is usually raised. This is an indication that your body is fighting an inflammation.
Why Do I Need These Tests?
When it comes to diagnosing a medical condition, one or a collection of symptoms can have many causes.
For example in AS, the most common presentation is pelvic (sacroiliac) joint pain from inflammation of the sacroiliac joint. Sacroiliitis (inflammation of the sacroiliac joint) can have many causes.
It can be caused by Psoriatic arthritis, Reiter’s syndrome, Ulcerative colitis or infection, to mention a few.
But by doing various tests one or the other condition can be ruled out. This is of course important so the most appropriate treatment can be given.
Chiropractic Treatment Of Ankylosing Spondylitis (AS)
The treatment includes nonsteroidal anti-inflammatory medication and physical therapy.
The chiropractor will show you exercises designed to strengthen your back, improve posture, increase flexibility, range of motion, and techniques to improve your breathing. We normally also use spinal manipulation of a kind that is safe and comfortable for you.
Because chiropractors specialize in treatment of lower back pain and usually have X-ray facilities on-site we often pick up when patients have AS early on.
Unfortunately, in some cases patients in past have been told by their medical practitioner that chiropractic treatment is not appropriate for them. But it is important to know that chiropractic treatment is a very helpful, safe and effective way of managing your AS.
We have had several patients over the years that have found that chiropractic treatment has maintained their mobility, improved their function and therefore helped to control their pain.
There is no doubt that anti-inflammatory medication will help if the inflammation is particularly bad. So, ideally you should be co-managed. Which means that your GP and/or rheumatologist and chiropractor should both be involved.
At the Isis Chiropractic Clinics we encourage co-operation between medical and complementary practitioners to give you the best possible care.
Here is some research for you if you want to read further.
Links to research
Research Link 1: Ankylosing Spondylitis and Chiropractic Care.
Research Link 2: Ankylosing Spondylitis and Chiropractic Care.
- high-purine foods anchovies
- organ meats
- bouillon
- gravies
- seafood
- goose
- yeast (baker’s and brewer’s)
- sweetbreads
Restricted Foods
- foods with moderate purine content
- fish
- meat
- poultry
- asparagus
- beans
- lentils
- diuretics
- alcohol
- niacin
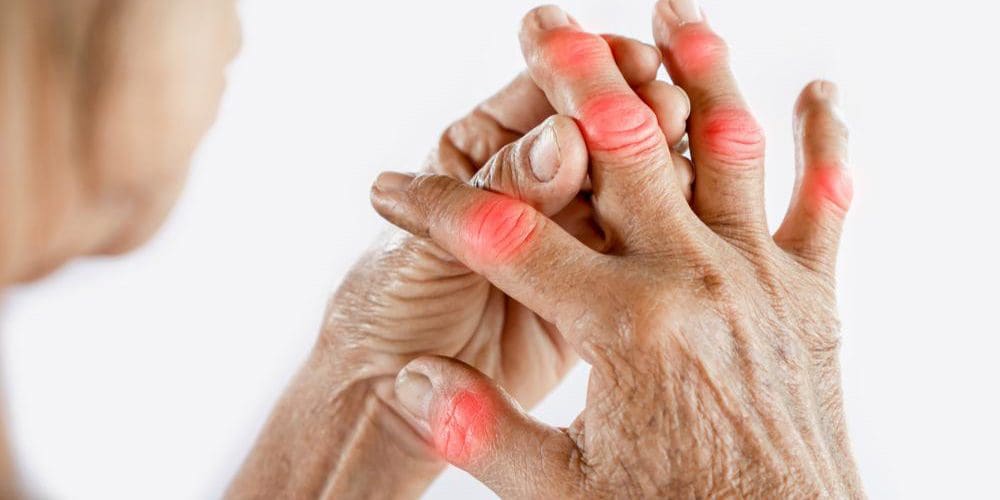
Chiropractic Care for Gout Pain
Chiropractic care may help reduce gout symptoms in multiple ways. The primary benefit of chiropractic care is that it helps to improve joint range of motion and flexibility and reduces pain. Chiropractic manipulation can also reduce inflammation, which helps alleviate the swelling associated with gout attacks. Furthermore, chiropractic care can help to release the built-up uric acid within the affected joint, which is one of the main causes of gout. Lastly, chiropractors are trained to identify and address any underlying issues contributing to your gout flare-ups, such as poor posture or muscle strength.Understanding Gout
Gout is an inflammatory arthritis caused by the deposition of monosodium urate crystals (MSU) in the synovial fluid and other tissues. Hyperuricaemia is correlated with gout incidence and recurrence.1 Gout usually presents as monoarticular and is more likely to affect the distal joints, most frequently the first metatarsophalangeal joint, ankle, and mid-foot, however it may also affect the hands, wrists, elbows, knees, hips and spine. Polyarticular gout is typically associated with chronic gout symptoms.2
The prevalence of gout worldwide is estimated to be 1–4%. It is more common in men (3:1 to 10:1) and older age groups, and is increasing in many developed countries (New Zealand, Canada, United Kingdom, Korea).3–5 In 2017, the greatest point prevalence estimates for gout were in New Zealand, Australia and the United States of America (US).5 In the US, general gout prevalence is 5.2% in males and 2.7% in females.6 With age greater than 80 years the prevalence increases to 9% in men and 6% in women. Prevalence of hyperuricaemia remained stable in the US from 2007–2016. However, Chen-Xu et al.7 propose that a new wave of rising obesity in younger age groups may lag a future increase in gout prevalence. It is suspected that Western diets, sedentary lifestyle, an increased frequency of obesity and hypertension are contributing factors to raised uric acid levels. Spinal gout, once thought to be a rare condition, may be more common than previously appreciated. Spinal gout has been identified in 14 to 29% of patients with a confirmed diagnosis of extremity gout.8–10 Prevalence may be significantly underestimated as only patients with severe symptoms, such as neurological deficit and fever, or those failing to respond to other therapies are investigated further.11 Advancements in imaging technologies such as Computed Tomography (CT), Magnetic Resonance Imaging (MRI) and Dual Energy Computed Tomography (DECT) have significantly improved the detection of spinal gout. DECT is an emerging technology designed to detect the presence of MSU crystalline deposits. The technology is well established for assisting with the diagnosis of extremity gout but is yet to be commonly utilized for detecting spinal gout. Several case reports summarized in our paper mention DECT as an important diagnostic tool for confirming spinal gout.12–14In this paper we analyse 38 case reports of spinal gout from between 2017 and 2022. Consistent with previous reviews, a high proportion (76%) of cases of spinal gout proceed to surgery with diagnosis only confirmed after excision and lab analysis.15–17 This highlights the need for earlier and less invasive detection methods for spinal gout, with particular application in primary care settings. In this paper we review advances in clinical diagnosis and imaging and recommend tools to improve recognition and earlier diagnosis of spinal gout.
Gout is a type of inflammatory arthritis caused by the buildup of uric acid in the blood. It happens when too much uric acid accumulates and forms urate crystals deposited in the joints and surrounding tissues. Gout can be treated with lifestyle modifications, medications, and other treatments. Proper medical care is essential to reduce the risk of long-term complications such as joint or organ damage.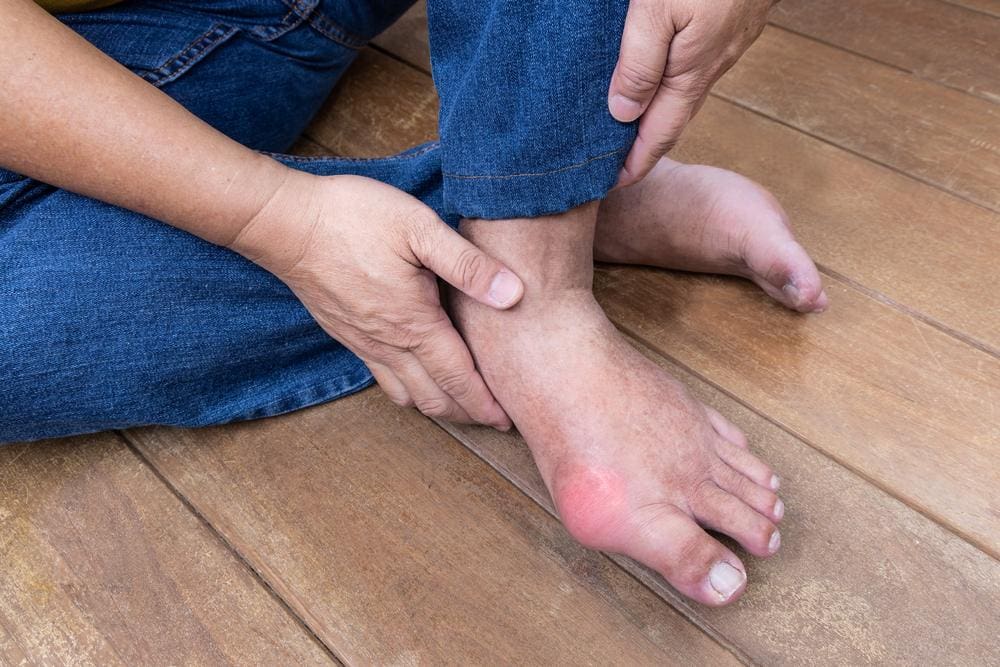
Causes
Gout is a complex disorder caused by multiple factors. Understanding the potential causes of gout is essential to start an effective treatment plan with your doctor. The most common cause of gout is the buildup of uric acid in the blood (hyperuricemia). Uric acid is created when purines, found in certain foods and drinks, are broken down in the body. Other causes include genetics, obesity, age, kidney disease, high blood pressure, certain medications, and excessive alcohol consumption. In some cases, the cause of gout is unknown.Symptoms
Gout can cause a variety of symptoms, including:- Sudden and severe joint pain
- Redness and swelling in the affected area
- Stiff joints
- Limited range of motion
- Heat sensitivity in the joints
- Fatigue
- Fever
Natural Gout Relief with Chiropractic Care
Chiropractic treatment can offer natural relief of gout symptoms. This is because chiropractic focuses on addressing the underlying cause of the discomfort associated with gout.
Chiropractic Treatments for Gout Pain
Chiropractors use various treatments to treat gout, including adjustments, soft tissue techniques such as massage, and nutritional guidance. Adjustments involve realigning the spine to reduce inflammation and improve overall function. Soft tissue techniques can help break down scar tissue or adhesions that may be causing severe pain or restricting the range of motion. Nutritional guidance helps patients identify dietary habits that may play a role in their gout flare-ups and how to make adjustments. Additionally, many chiropractors will provide lifestyle advice on managing stress levels, getting regular exercise, and practicing relaxation techniques such as yoga or tai chi.Gout Relief At Home
You can use at-home treatments for gout to reduce symptoms and decrease the amount of time you suffer from an episode. These treatments often focus on lifestyle changes, such as following a diet low in purines, drinking plenty of fluids, and exercising regularly. There are some natural methods to treat gout symptoms. Some foods and supplements may help reduce inflammation and lower uric acid levels in the body. Certain foods and herbs that contain anti-inflammatory properties are beneficial in reducing swelling, stiffness, and pain associated with gout. These include:- Cherries and tart cherry juice
- Dark-colored fruits and vegetables such as blueberries
- Foods high in omega-3 fatty acids
- Garlic
- Turmeric
- Feverfew

Conclusion
Once you have narrowed your search and decided to consult a chiropractor, there are some crucial factors to consider before making an appointment. It is essential to choose a qualified professional that is experienced in treating gout. Ask for referrals from friends and family who have consulted with a chiropractor to treat their gout, as this can be a great way to find the most qualified practitioner. You should also research chiropractors and read online reviews from past patients. Once you have identified a few practitioners who meet your criteria, you can contact them directly and inquire about their experience treating gout. Ask questions such as:- How many patients have they treated for gout?
- What techniques do they use to help relieve the symptoms of gout?
- Are there any additional services or treatments that could help manage my condition?
Tab Content
Tab Content
Tab Content
Gout is an extremely painful
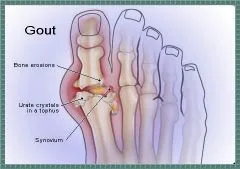
An estimated 840 out of 100,000 people, usually between the ages of 30 and 50, get gout. It is 20 times more common among men than women. Women rarely get gout before the onset of menopause. Some families are genetically predisposed, and African-Americans as well as individuals with poor kidney function are more likely to suffer gout attacks.
According to the 2007-2008 National Health and Nutrition Examination Survey (NHANES), gout affects upwards of 3.9 percent of the American population, and hyperuricemia (an excess of uric acid in the blood, which is a precursor to gout) affect 21.5 percent. The typical western lifestyle is also blamed for the increased incidence of the disease.
Recurrent bouts of gout can lead to “gouty arthritis,” which is a degenerative type of chronic arthritis. Some common medications, such as diuretics, may also contribute to gouty arthritis.
Types of Gout:
- Primary Gout is a genetic disorder of uric acid metabolism leading to high levels of serum uric acid. High serum uric acid levels cause monosodium urate crystals to precipitate out of solution into a joint, usually only one at a time, at least in the early stages of the disease. The presence of urate crystals in a joint sets off an immune response which causes the body to attack the internal components of the joint, leading to extreme pain and eventually joint destruction.
- Secondary Gout (10% of cases) results from catabolism secondary to leukemias and certain other cancers, or decreased excretion of uric acid due to renal failure. Uric acid rate of solubility is greatly affected by temperature, which is why the majority of cases present in a distal extremity. It is thought that the crystals also have a tendency to form on a roughened surface, such as a joint that has suffered from previous trauma, unreduced subluxation, or degeneration.
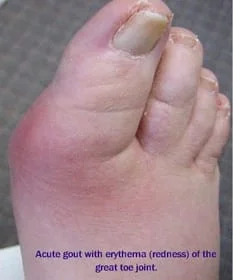
Gout is caused by elevated blood levels of uric acid, a waste product of the breakdown of cells and proteins. This excess can be due to an increase in uric acid production as well as the inability of the kidneys to adequately clear uric acid from the body. Certain foods, such as shellfish, and excessive consumption of alcoholic beverages may increase uric acid levels and precipitate gout attacks. Obesity, hypertension, diabetes, and medications can also increase uric acid levels. With time, the elevated levels of uric acid in the blood may form needle-like crystals in the joints, leading to acute and very painful gout attacks. Uric acid may also collect under the skin, which is known as tophi or in the urinary tract as kidney stones.
What are the Symptoms of Gout?
The most common symptoms of gout are insidious episodes of extreme pain without any trauma, inflammation, swelling (edema), tenderness, warmth and redness in the affected distal joint or extremity… usually in the big toe (the first metatarsophalangeal joint) which accounts of up to 60% of initial attacks.
Touching or moving the affected joint is intensely painful, and patients often say it hurts to have as little as a bed sheet over the affected joint. The pain may be accompanied by a mild fever. Gout develops quickly, and although it typically occurs in only one joint at a time, on rare occasions symptoms may develop in two or three joints simultaneously. In most cases, however, if these symptoms occur in joints throughout the body, the condition is probably not gout.
History may also reveal a high-purine diet; an excessive intake of alcohol (particularly beer); the use of diuretics; the use of aspirin; the low intake of water; a very reduced caloric intake (leading to catabolism); or a family history of gout, diabetes, hypertension and obesity are some pre-disposing factors. Signs include tophi deposits at the helix of the ears and high serum uric acid levels, not necessarily above the high range listed on a lab report. Levels over 6 mg/dL may be symptomatic.
How does chiropractic help gout?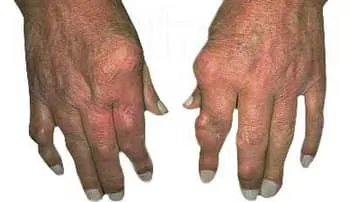
The most common medical approach to treating gout is to prescribe medications, anti-inflammatory drugs and steroids to manage pain. While this may work on a short-term basis, it may also cause unwanted drug-related side effects. In contrast, the chiropractic treatment of gout usually involves a combination of advice about diet and lifestyle changes along with chiropractic adjustment/manipulation to reduce pain and address the cause of the disease without the use of drugs.
We know the nervous system (brain, spinal cord, and nerves) is the master control system of the body. It controls every organ, muscle, gland, etc. at all times. If for example your kidneys don`t receive the right nerve supply from the brain, they will not function properly anymore. This could happen due to a misaligned vertebra (Vertebral Subluxation) in the lower back. This doesn`t need to cause any pain, but over time altered neurological control to the kidneys may have an effect on the kidneys in that they may not adequately eliminate the uric acid in the body. This uric acid would then form crystals at a particular spinal segment or joint, and the symptoms of gout would set in (painful red-shiny joint). Correcting these spinal or joint misalignment problems through a chiropractic adjustment/manipulation is the job of a chiropractor.
Your chiropractor will likely advise that you reduce your intake of meat and alcohol and increase your intake of foods that have been shown to lower the concentration of uric acid in the blood, such as cherries. Half a pound of cherries per day is the recommended amount to eat if you are looking to lower uric acid levels. However, you can also drink concentrated cherry juice or take cherry juice extract to achieve the same results if cherries are out of season or eating that many is not to your taste. Quercetin, a flavonoid found in such foods as apples, berries and onions, inhibits the production of uric acid, so your chiropractor may also suggest that you include more of these in your diet as well. Herbs that support kidney function (like couch grass) may also be recommended; since they may help your kidneys work more efficiently to clear the blood of excess uric acid.
In combination with these, your chiropractor may perform adjustments or manipulations along with using low level laser therapy, heat and/or ultrasound and corrective stretches and exercises to help bring the body back into alignment and relieve pain
Chiropractic care is an effective way to manage gout. Chiropractors are able to help relieve any subluxations (mis-aligned vertebrae pinching nerves) in your spine that may be interfering with the communication between your nervous system and brain, including body tissues. The nervous system controls all the organs of the body, including the kidneys. If the kidneys aren’t getting the proper nerve supply from the brain it will cease to work properly. In this way, specialized chiropractic techniques performed by your chiropractor can help the kidneys begin to function properly again.
In addition to providing you with adjustments, Dr. Pisarek can teach you ways to manage your gout when you’re not in the office. One of the best things that a patient with gout can do is to eat a diet that’s low in purines. Another is to ensure that you’re getting enough of foods that have natural anti-inflammatory properties.
Other Treatment Options for Gout:
Conventional medical treatments may help relieve the symptoms of gout, but they do not address the root of the problem. By strengthening structural weaknesses and addressing imbalances in the body, as natural treatments such as with chiropractic care, pain associated with gout may be alleviated permanently.
- The allopathic (medical) drug of choice for the treatment of gout is allopurinol. Although effective in reducing serum uric acid levels, allopurinol may precipitate over 30 adverse side effects, including abdominal pain, hepatitis, headache, kidney failure, hair loss, muscle disease and joint pain. The most common side effect is a sometimes fatal skin reaction in which one’s skin peels off in sheets.
- The natural approach to the treatment of gout includes counseling the patient on dietary changes, with a reduction of high-purine foods, increased consumption of water (at least 64 ounces per day), along with 12-16 ounces of cherry juice per day and the elimination of alcohol, especially beer. Aspirin should be avoided, as it raises uric acid levels. Over-the-counter (OTC) medications such as Aleve may be substituted, as it lowers uric acid levels, but it can cause stomach problems. In the acute and chronic stages, laser, ultrasound, heat, gentle chiropractic manipulative therapy and gentle soft-tissue massage are beneficial.
Click here for article “The 5 Steps to Overcoming Gout Naturally”
What foods are preferred?
- Foods that might possess anti-inflammatory benefits and are rich in Vitamin C such as fresh bing cherries and natural cherry juice
- Berries, pineapple, bananas, oranges, tomatoes
- Green-leafy vegetables, kale, cabbage, celery, parsley, tomatoes, potatoes
- Red cabbage, tangerines, red bell peppers, mandarins
- Low-fat dairy products; Tofu
- Complex carbohydrates (breads, rice, pasta)
- Essential fatty acids (salmon, tuna, flaxseed, olive oil, nuts, seeds).
All of these foods are healthy ways to reduce inflammation in your body without resorting to NSAIDs. In addition to eating anti-inflammatory foods, certain lifestyle changes may be in order if you wish to reduce your gout symptoms. Managing your weight, limiting your alcohol consumption and increasing your level of exercise are all great ways to manage gout. They can also help lower your risks for developing gout in the future.
What foods should be avoided? Alcohol, Anchovies, mussels, herring, sardines, scallops, meat extracts, yeast, gravies, organ meat (hearts, kidneys, liver), Goose, Pheasant and Trout.
The following foods are considered high in purines as well, but may not raise the risk of gout: asparagus, spinach, cauliflower, peas, kidney and lima beans; mushrooms; cereals, breads; chicken, duck, ham, and turkey.
Remember: Protein should not be totally eliminated in ones diet, even though purines are found in all protein rich foods.
Foods to Avoid:
- high-purine foods
- organ meats
- bouillon
- gravies
- seafood
- lentils
- goose
- yeast (baker’s and brewer’s)
- sweetbreads
- mushrooms
- beer
Restricted Foods:
- foods with moderate purine content
- fish
- meat
- poultry
- asparagus
- beans
- lentils
Also Avoid the Following:
- diuretics
- alcohol, especially beer
- niacin





